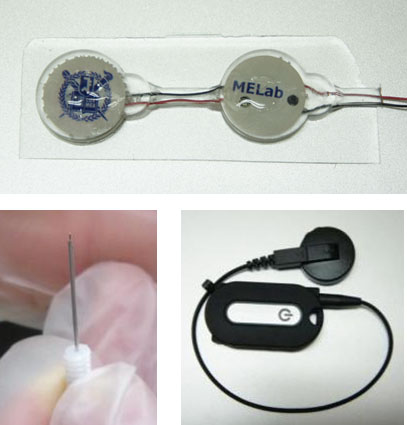
Neural Prosthesis & FES in MELab
Paralyzed or paretic muscles can be made to contract by applying electrical
currents to the intact peripheral motor nerves innervating them. When electrically
elicited muscle contractions are coordinated in a manner that provides function, the
technique is termed functional electrical stimulation (FES). In more than 40 years
of FES research, principles for safe stimulation of neuromuscular tissue have been
established, and methods for modulating the strength of electrically induced muscle
contractions have been discovered. FES systems have been developed for restoring
function in the upper extremity, lower extremity, bladder and bowel, and respiratory
system. Some of these neuroprostheses have become commercialized products, and
others are available in clinical research settings. Technological developments are expected
to produce new systems that have no external components, are expandable to
multiple applications, are upgradable to new advances, and are controlled by a combination
of signals, including biopotential signals from nerve, muscle, and the brain.
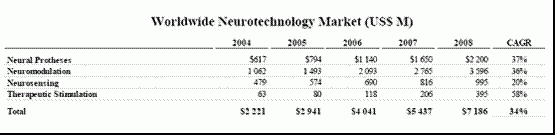
<Worldwide Neurotechnology Market>
Ongoing Project
DBS (Deep Brain Stimulator)
Developed system for preclinical test
Deep Brain Stimulation(DBS), one form of neural prostheses, has been introduced first by Grenoble group in 1980s.1), During the last decade, DBS of the Subthalamic Nucleus (STN) emerged to the most frequently applied surgical therapy for movement disorders, representing a most promising breakthrough in the treatment of advanced PD. Following pioneering works showing striking improvements in PD patient’s motor function and quality of life, an increasing number of groups started to use DBS worldwide as a routine method for treatment of advanced PD. Medtronic first diveloped commercial DBS implanted system, Activa® Therapy, in 1996 and now more than 30,000 patients worldwide are implanted Medtronic's DBS system.2) However, as the mechanism of the action of DBS has not been elicited perfectly yet and thus the data from High freqeuncy deep brain stimulation(HFS) on 6-hydroxydopamine (6-OHDA) induced animal PD models can contribute to understand the mechanism. In our lab, implantable DBS system for a rat PD model is developed for long term study experiments are in progress.
Elapsed Project
Diaphragmatic Breathing Pacemaker
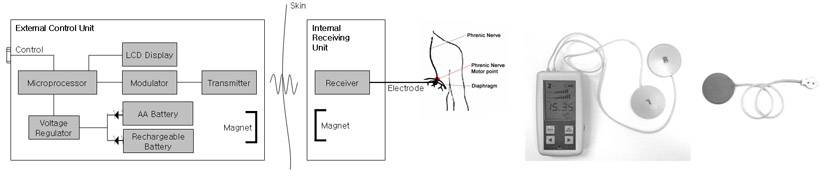
The number of patients with high cervical spinal cord injury(SCI) is 500,000 world-widely (250,000 in US). Mechanical ventilator has many disadvantages (e.g. physical discomport, difficulty with speech, mortality, impaired sense of smell and so forth) and phrenic nerve pacing carries some risk of injury to the phrenic nerves. So Diaphragmatic Breathing Pacemaker (DBP) can be an appropriate solution where transmission coils are located on the skin of the breast.
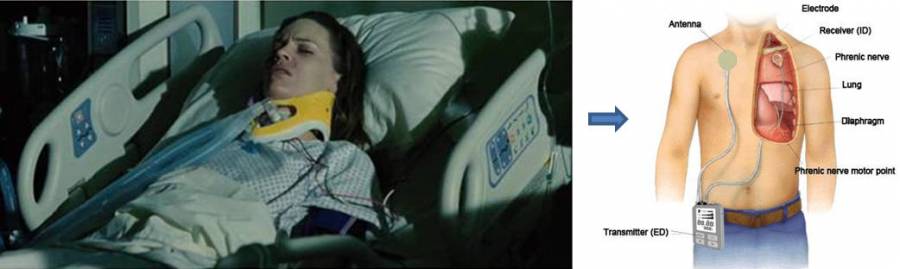
<For Cervical Spinal Cord Injury (in Million Dollar Baby, 2004)>
Breathing pacemaker that uses a minimally invasive laparoscopic procedure to position intramuscular electrods bilaterally near the motor point of the diaphragm, can be an alterative to direct stimulation of the phrenic nerve. The connection between ECU (external control unit) and IRU (Internal receiving unit) uses transcutaneous energy transmission (TET). Recently, coil design for more efficient enery trnasmission, detection of self respiration and synchronization of stimulation are in progress.